Health
The health of our nation and the South as a region hinges significantly on how well we address and reduce health disparities among groups that bear a disproportionate burden of illness, disability, and mortality. Studies have shown that Southerners are more likely than those in the rest of the nation to have certain chronic illnesses and to experience worse health outcomes. According to the Kaiser Family Foundation, one in five (20%) adults living in the South reports fair or poor health status, compared to 16% of adults in the Midwest and Northeast and 17% of adults in the West.
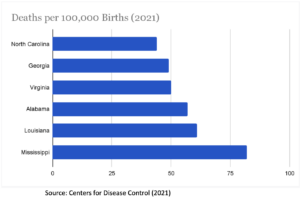
Adding to an already-troubling statistical representation of the health of the region are the new challenges related to reproductive rights and freedoms for pregnant people. Restricted abortion access in the South has a disproportionate impact on women in the region and contributes to higher maternal morbidity rates. According to the CDC, in 2020 the United States had a maternal morbidity rate of 23.8 deaths per 100,000 births, with over 80% of those deaths being preventable. In 2021, the six states with the highest maternal morbidity rates were in the South: Mississippi (82 deaths per 100,000), Louisiana (61 deaths per 100,000 births), Georgia (49 deaths per 100,000 births), Alabama (57 deaths per 100,000 births), North Carolina (44 deaths per 100,000 births), and Virginia (50 death per 100,000 births). It must be noted that these six states also had some of the highest shares of Black births in the country.
The 2023 legislative sessions were the first full sessions to convene post-Dobbs v. Jackson and many anticipated that the measures that would emerge from these sessions would undoubtedly be extreme, given the U.S. Supreme Court’s return of regulation of abortion to the states. During the sessions, state legislative bodies across the South reckoned with the post-Dobbs landscape. While there were several bills seeking to impose bans and limit access to reproductive health care, many legislators proposed legislation to provide more equitable access to health services, such as prenatal and postnatal care, doula access, and maternal mortality research.
Because of the prevalence and presence of this issue in the 13 state legislature, EPU’s focus for this Health section of the 2023 Southern Legislative Wrap up is on those bills related to maternal health disparities and the efforts to mitigate the anticipated consequences of limiting or restricting reproductive health freedoms in this country. The legislation detailed below provides examples of ways that legislators sought – both successfully and unsuccessfully – to ensure the health and safety of pregnant people pre- and post-birth and secure the right of the privacy of an individual to make reproductive choices and have access to a basic level of quality, affordable, and informed health care.
We are proud of the work of our Unum Fellows from Cohort 2 who have both supported and championed efforts related to maternal health care, including Rep. Park Cannon (Georgia), Representative Aimee Freeman (Louisiana), Rep. Kim Schofield (Georgia), and Rep. Harold Love, Jr. (Tennessee).
Prenatal and Postnatal Care
Access to prenatal and postnatal care is essential for addressing maternal health disparities for several reasons.
Prenatal care allows providers to identify and address potential health risks and complications early in pregnancy, which can mitigate risks and improve maternal and fetal outcomes. Women in marginalized communities often face a higher risk of pregnancy complications and adequate prenatal care allows healthcare workers to monitor high-risk pregnancies more closely, reducing the likelihood of adverse events and ensuring appropriate medical intervention. Postnatal support is equally important for monitoring the health of both the mother and the newborn child after birth. Ongoing care can help detect and address postpartum complications.
Many maternal health outcomes can be prevented or managed with proper care. Access to prenatal and postnatal care reduces the likelihood of complications such as preterm birth, low birth weight, and postpartum depression, which disproportionately affect marginalized communities.
The bills below serve as a few examples of legislation from the 2023 sessions aimed at ensuring the availability and enhancement of prenatal and postnatal care for pregnant people in the South.
- South Carolina Senate Bill 29 (failed) – Aimed at amending various aspects of reproductive healthcare in South Carolina, this bill proposed allowing women to have abortions before the viability of the embryo or fetus, outlined circumstances for abortions after viability, permitted doctors to prescribe abortion-inducing drugs through telemedicine, and mandated health insurance policies to cover abortions and related services
- Georgia House Bill 129 (enacted) – Expands Temporary Assistance for Needy Families (TANF) eligibility criteria to include pregnant women
- Why it’s important: Expanding TANF eligibility to pregnant people is vital to ensure their access to essential prenatal care and reduce financial stress during a critical period. This support not only promotes healthier pregnancies and birth outcomes but also contributes to long-term maternal and child well-being.
- Virginia House Bill 1531 (enacted) – Convenes a working group to collaborate on strategies to improve care for mothers and children.
- Why it’s important: Bringing together diverse expertise and perspectives to address complex healthcare challenges is an important step toward developing innovative solutions and ensuring that systems are better equipped to provide high-quality care for the well-being of mothers and children.
Doula Access
Birth doulas provide emotional, physical, and informational support to expectant mothers before, during, and after childbirth. Doulas serve as advocates for the birthin person’s wishes and preferences. They ensure that the birth plan is communicated to healthcare providers and is respected. They also provide evidence-based information about labor and childbirth options, procedures, and interventions, empowering pregnant people to make informed decisions and understand risks and benefits of certain choices.
During the birthing process, they can provide a calming presence, offer reassurance, and help people to cope with the emotional challenges of labor and childbirth. They also assist with comfort measures during labor, such as helping with positioning, massage, and breathing techniques. While the primary focus is on labor and birth, many doulas also offer postpartum support.
There is growing evidence that the use of doulas during the pregnancy and birthing process is paramount in reducing maternal morbidity, particularly for pregnant people of color who face disproportionate risks. Studies show that women of color face systemic biases and disparities and experience significantly higher rates of systemic maternal morbidity compared to their white counterparts. According to the Centers for Disease Control and Prevention, Black women are three times more likely to die from pregnancy-related causes than white women.
While birth doulas offer valuable support, they are not medical professionals and do not provide medical or clinical care, diagnose medical conditions, or perform medical procedures. Instead, they complement the care provided by healthcare providers by offering holistic, non-medical support to enhance the birthing experience and promote positive outcomes. This is important to note because doula services are often not covered by insurance providers or Medicaid programs because they serve in a non-medical role. This landscape is evolving, however, as some insurance providers and Medicaid programs in certain states are beginning to explore and pilot programs that cover doula services.
By providing emotional, physical, and informational support, doulas play a critical role in addressing these disparities. They offer continuous advocacy, emotional support, and evidence-based care, which have been shown to positively impact maternal outcomes and help mitigate the racial disparities in maternal health. By offering personalized support and guidance, doulas empower women of color to make informed decisions about their pregnancies and birthing experiences, ultimately contributing to improved maternal and infant well-being.
The bills below serve as a few examples of legislation from the 2023 sessions aimed at exploring and incorporating the use of doulas in the standard of care for maternal health care in the South.
- Tennessee HB 576 (and companion bill SB 128 – failed) – These bills sought to require TennCare (the state Medicaid program) to create a pilot program to pay for doula services for pregnant people who meet certain criteria for up to 12 months postpartum. Criteria included a determination of increased likelihood for a high-risk pregnancy and lack of reliable transportation to access a healthcare provider.
- Why it’s important: Legislation that acknowledges and addresses barriers faced by marginalized communities is essential for promoting equity. By including provisions that allocated additional resources to overcome these barriers or that recognize the risks that are elevated by these barriers (such as lack of reliable transportation), lawmakers can actively work to level the playing field and ensure that all members of society have a fair chance to access opportunities, and in this case, have a fair chance at survival.
- Tennessee HB 738 (and companion bill SB 187 – enacted) – Rep. Harold Love, Jr., one of the members of Cohort 2 of our Unum Fellows program, successfully enacted this legislation which creates a doula services advisory committee, tasked with establishing core competencies for doulas across the state and recommending reimbursement rates and fee schedules for medicaid reimbursement of doula services.
- Why it’s important: Much like with convening of the working group in Virginia to study strategies for improving the health of mothers and children, creating this type of group is critical to ensure quality doula care for expectant mothers, particularly in marginalized communities. It not only promotes equitable access to this valuable support but also addresses maternal health disparities and infant health outcomes while potentially leading to cost savings in the healthcare system.
Maternal Health and Mortality Research
Researching and studying maternal health and mortality serves as the cornerstone for enhancing maternal health outcomes. Through research requested and provided to state legislatures, those charged with legislating on our behalf have the ability to gain a comprehensive understanding of the factors influencing maternal mortality. This knowledge can empower healthcare professionals and policymakers to develop evidence-based strategies and interventions, removing rhetoric from the conversation to lead to improved care, reduced risks, and saved lives.
This type of objective research also plays a pivotal role in addressing disparities in maternal outcomes, which is pivotal for achieving health equity. Armed with this data, policymakers should be forced to direct interventions and allocate resources where they are needed most, ensuring that all pregnant people have equitable access to high-quality maternal care.
As with the other trends we saw related to maternal health in the 2023 legislative sessions, legislation brought forward regarding the research of maternal health and mortality also varied in its success. Below are a few examples:
- Texas HB 1664 (failed) – This bill specifically sought to study maternal mortality and morbidity among Black women in the state.
- Virginia SB 1254 (enacted) – This bill amends the current law concerning the Maternal Mortality Review Team, changing the frequency of their compilation, comparison, and release of statistical data about maternal mortality in Virginia from once every three years to annually.
- Louisiana Senate Concurrent Resolution 20 (enacted) – This bill creates a task force to make recommendations about the involvement of nurses to improve maternal outcomes.
2024 Outlook
When women face barriers to accessing safe and legal abortion services, they may resort to unsafe or delayed procedures, which can lead to serious health complications. These complications can, in turn, increase the risk of maternal morbidity, including infections, hemorrhage, and long-term health issues. Limited access to abortion services exacerbates maternal health disparities in the South, particularly for low-income women and women of color, as they may face additional challenges in obtaining timely and appropriate reproductive healthcare.
The progress in the health equity space has been varied – especially as it relates to maternal health – letting us know that there is still much work ahead to ensure that every individual, regardless of identity, appearance, or location, receives the best possible healthcare. State legislatures must focus in 2024 on continuing to advance legislation aimed at reducing healthcare access disparities and improving outcomes, including pregnant people who may no longer have the choice to decide whether to give birth based on the reproductive laws in their state.
